دیابت و عوارض آن
دیابت به روشهای مختلفی میتواند منجر به ایجاد آسیبهای قلبی- عروقی شود. این فرآیندها به طور مستقل پیشرفت نمیکنند بلکه هر کدام ممکن است منجر به بدتر شدن دیگر فرآیندها شوند. بدین معنی که وقتی فردِ مبتلا به دیابت دچار سکتۀ قلبی میشود، پیشبینی مراحل بیماری نسبت به دیگر افراد سختتر است. این امر به دلیل ایجاد چرخۀ معیوب ناشی از اختلالات عروقی ترکیبی مرتبط با بیماری دیابت میباشد.
اختلالات عروقی ممکن است بسیار جدی و نگران کننده باشد چرا که آسیب به عروق خونی میتواند منجر به عواقبی از جمله سکته مغزی و از دست دادن اندامهای بدن شود.
همۀ انواع دیابت منجر به بیماری سیستم قلب و گردش خون میشود. دو فرآیند اصلی در دیابت که باعث ایجاد آسیبهای پیشرونده در قلب و عروق خونی میشوند شامل تصلب شرائین (Atherosclerosis) و فشار خون بالا (Hypertension) است.
از آنجا که تصلب شرائین، عروق خونی متوسط و بزرگ را درگیر میکند، اغلب از عبارت ماکروآنژیوپاتی برای نشان دادن این مشکل در افراد مبتلا به دیابت استفاده میشود.
ماکروآنژیوپاتی بیماری مربوط به عروق خونی بزرگ است که در آن چربی و لختههای خون ایجاد شده به دیوارۀ عروق میچسبند و موجب انسداد جریان خون میشوند. انواع ماکروآنژیوپاتی شامل بیماری عروق کرونر (ماکروآنژیوپاتی در قلب)، بیماری عروق مغزی (ماکروآنژیوپاتی در مغز) و بیماری عروق محیطی (ماکروآنژیوپاتی در عروق پاها) است.
علاوه بر تصلب شرائین (ماکروآنژیوپاتی)، یکی دیگر از مشکلات مرتبط با دیابت، میکروآنژیوپاتی است.
میکروآنژیوپاتی بیماری مربوط به عروق خونی کوچک است که در آن دیوارۀ عروق بسیار ضخیم و ضعیف میشود به طوری که موجب خونریزی و کاهش جریان خون خواهد شد. اثر میکروآنژیوپاتی بر عملکرد مویرگی منجر به کاهش انتقال اکسیژن و مواد مغذی به بافت و نشت پروتئین به فضاهای میان بافتی میشود.
یکی از بدنامترین شکلهای میکروآنژیوپاتی، در بیماران مبتلا به دیابت کنترل نشده یافت میشود. کاهش جریان خون منجر به کاهش اکسیژنرسانی به بافت شده و این امر میتواند باعث نکروزه شدن بافت یا اندام گردد. به عنوان مثال ممکن است بخشی از بافت پا بمیرد و آسیب ایجاد شده به طور بالقوه منجر به قطع عضو شود چرا که با مرگ بافت امکان احیا کردن آن وجود ندارد.
افراد مبتلا به دیابت ممکن است در بسیاری از نقاط بدن مانند چشمها دچار میکروآنژیوپاتی شوند. میکروآنژیوپاتی بر مویرگهای سراسر بدن اثر میگذارد اما آسیب به مویرگهای گردش خون در چشمها، کلیهها و اعصاب بیشتر باعث ایجاد تظاهرات بالینی در بدن میشود که از جمله آنها میتوان به رتینوپاتی، نفروپاتی، نوروپاتی و پای دیابتی اشاره نمود.
میکروآنژیوپاتی ممکن است در سیستم اعصاب مرکزی نیز ایجاد شود و منجر به سکته گردد. مغز به طور خاص در برابر وقفه در اکسیژنرسانی بسیار آسیبپذیر است. اگر جریان خون به مغز مختل شده یا کاهش یابد، سلولهای مغزی میمیرند. بسته به ناحیهای از مغز که درگیر میشود، بیمار علائم مختلفی خواهد داشت.
از طرفی دیابت میتواند بر اجزای مختلف سیستم عصبی نیز اثر بگذارد. آسیب به اعصابی که اندامهای داخلی بدن شامل قلب و عروق خونی را عصبدهی میکنند، به نام نوروپاتی شناخته میشود. همانطور که بیان شد، نوروپاتی میتواند به دنبال میکروآنژیوپاتی عروق کوچک ایجاد شود.
از بین رفتن عصبدهی عروق خونی کوچک همچنین ممکن است تنظیم جریان خون را مختل کند و این یک عامل مهم در توسعۀ زخم پای دیابتی است.
درمان عوارض دیابت
سیستم سمپاتیک در مقابل سیستم پاراسمپاتیک قرار دارد. یکی از وظایف سیستم سمپاتیک ترشح هورمون آدرنالین در مواقع بحرانی است که باعث افزایش ضربان قلب و فشار خون میگردد اما یکی از وظایف خاص دیگری که بر عهده دارد، انقباض عروق محیطی و کاهش جریان خون در اندامها است.
عصبهای سمپاتیک بخشی از سیستم اعصاب سمپاتیک هستند که در دو طرف نخاع و در بخش پایینی پشت قرار گرفتهاند. قبلاً جهت درمان اختلالات سیستم سمپاتیک (همچون بهبود جریان خون اندامها در بیماری برگر و دیابت) از روش جراحی و بیهوشی عمومی برای بلوک سمپاتیک (سمپاتکتومی) استفاده میشد که همراه با عوارض بود. اخیراً با پیشرفتهایی که در تکنیکهای اینترونشنال کنترل درد صورت گرفته است میتوان بدون نیاز به بیهوشی عمومی و جراحی باز این عمل را انجام داد.
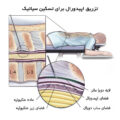
بلوک سمپاتیک کمری برای مسدود کردن اعصاب سمپاتیک که به سمت پاها میروند، به کار میرود. این روش با بیهوشی موضعی در داخل یا اطراف عصبهای سمپاتیک انجام میشود. بلوک سمپاتیک کمری ممکن است جهت کاهش درد، تورم، تغییر رنگ، تعریق شدید و یا دیگر تغییرات غیر معمول در اندام پایین تنه به کار رود. همچنین این روش میتواند به منظور درمان مشکلات عروقی، عصبی و زخمهای دیابتی در افراد مبتلا به دیابت استفاده شود.
بلوک سمپاتیک کمری تحت شرایط استریل انجام میگیرد. پوست ناحیۀ پشت با محلول ضد عفونی کننده تمیز شده و سپس به صورت موضعی بیحس میشود. در مرحلۀ بعد پزشک از اشعۀ ایکس برای هدایت سوزنها در امتداد اعصاب سمپاتیک و قرارگیری آنها در موقعیتهای مناسب استفاده میکند. پس از تشخیص محل مناسب، حرارت ایجاد شده توسط امواج رادیویی با کمک این سوزنهای خاص به اعصاب سمپاتیک اعمال شده و موجب تخریب آنها میشود.
بیمار ممکن است بلافاصله پس از عمل در بخش پایین تنه احساس گرما کند. در محل اعمال سوزن نیز ممکن است کمی درد ایجاد شود اما از آنجا که این روش با حداقل تهاجم صورت میگیرد، زمان ریکاوری کوتاه است و بیمار میتواند پس از یک روز استراحت به فعالیتهای روزانه خود بازگردد.
با کمک خداوند متعال، عمل سمپاتکتومی قفسه سینه با امواج رادیویی بدون نیاز به بیهوشی و جراحی توراکوسکوپیک، جهت سمپاتکتومی کمری برای درمان نارسایی عروق شریانی اندام پایینتنه (در پای دیابتی و بیماری برگر)، برای اولین بار در ایران و برای دومین بار در سطح بینالملل توسط دکتر کامبیز باقرزادی با موفقیت و بدون عوارض انجام شده است.