Nonaggressive waist and cervical disk therapies:
One of the most prevalent reasons for waist and neck pains is the Intervertebral Disk Herniation (IDH) which is simply referred to as waist or neck disk. Some IDH cases can be treated by resting, physiotherapy and medical treatment. However in the case of majority of these cases, the mentioned therapies are not effective and the patient will need a surgery. Previously, the common therapy for IDH was open surgery which was so frightening for the patients because of its rather long treatment period and its potential side effects as well. However, nowadays as the technology has made progress, newer nonaggressive therapies including outpatient surgery have become more frequent. In the following some of these nonaggressive methods are described:
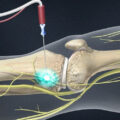
Intervertebral Disk Herniation (IDH): the disk is a soft padding in between the vertebras of the spinal cord and allows the vertebras to slide on each other so that the pressures on the spinal cord are adjusted. The inner part of the disk is a gelatin form material while the outer part is a rubber like material with flexibility. When there is exceeding pressure on the spinal cord, IDH occurs. In this case, the gelatin section of the disk gets displaced and so disk herniation happens. In more severe cases, the disk may get torn which is followed by more severe symptoms. IDH causes pressure on the nerves that exit the marrow. These nerves have different tasks. As an example the entire feelings of pain, touching of hands, legs and other parts of the body are transferred to the brain through these nerves. The disk’s pressure on these nerves can disrupt the tasks of these nerves or create pain, sensory side effects and motor side effects as well. IDH is commonly seen in waist vertebras and neck vertebras.
Nonaggressive IDH therapies:
ٍEpidural Corticosteroid Injection: the main cause of pain of IDH is not merely the pressure inflicted on the marrow, rather this pressure also creates severe inflammation in the proximity of the nerves and this by itself promotes more pain. Corticosteroid drugs are injected proximal to the nerves under pressure and they can reduce inflammation and will resultantly reduce pain significantly. As the pain reduces, it would become possible to attend to physiotherapy movements and through these exercises the vertebras’ positioning gets corrected and so the displaced disks may get back to their normal condition to some extent. In order to do this injection, not only the skin must be opened so that the needle could reach the spinal cord, but also the physician must use a tool that allows seeing the marrow behind the skin. This has become feasible by technology. By making use of a specific type of imagery tool commonly known as fluoroscopy, the surgeon cab clearly see the patient’s spinal cord and its surrounding tissues. Through a short outpatient surgery and through the application of topical anesthesia, the surgeon injects the Corticosteroid drug into a section of marrow known as the epidural space. This therapy has a very slight pain and the entire operation takes less than ten minutes. And also after being checked for vital signs, the patient will be dismissed. By this therapy, pain reduction usually takes place rapidly and a majority of patients can get back to their normal lives after one or two days. The injection may need to be repeated twice in one or two week intervals; however no more than three injections is recommended and for patients who experienced no pain reduction, the second injection will not be recommended.
Percutaneous Laser Disc Decompression (PLDD):
This surgery is a well-known therapy for IDH and it was for the first time done thirty years ago. The basis of this treatment relies on decompression of the displaced disk and returning it to its previous condition. In a condition similar to the formerly mentioned therapy the surgeon uses the fluoroscopy and then reflects a thin ray of laser light into the gelatin part of the disk through a long needle; this results in a controlled heat within the disk which evaporates the fluids within the disk to the extent needed; therefore the disk is pulled back inside and so the pressure on the marrow will be relieved. In addition this thermal effect may also repair the outer layer of the disk as well. This surgery is completed in less than 30 minutes and by it symptoms will be faded rapidly. Most patients who use this treatment will get back to their routine lives in less than a few days. The results of a 12 year study on 518 patients, shows a 75-89 percent rate of successfulness for this method with less than one percent of side effects. This method is also approved and certified by the FDA.
Ozone therapy: Ozone is a three-molecule oxygen gas with extreme effects when combined with the materials within the gelatin section of the disk. Through a method similar to the above mentioned methods and through the application of a long needle, the Ozone gas is injected into the disk and so when the fluids within the disk are evaporated, the disk gets back to its original condition and so the pressure on the marrow will be relieved.
Discogel Injection: in this method a special material is injected into the disk through a similar method. This material merges with gelatin and gets it out of its solid state and therefore, the disk’s out-moving capability gets minimized.
Hydro-Discectomy: hydro-discectomy is a roughly new nonaggressive therapy which uses high pressure water flow to remove the upper tissue of the displaced disk. By doing so the pressure inflicted on the marrow will be removed and so the patient’s pains will be gone.
In contrast to methods such as laser or radiofrequency which use a thermal mechanism for repairing the displaced disks, and also considering the high probability of infliction of tissue damage by lasers and radiofrequencies, the water pressure based discectomy method is free from heat stimulated tissue damage. In this method, high pressure water passes through the device and enters the disk; based on the venture law, a suction state is created which allows the disk particles to exit along with water flow.
In the end it must be added that diagnosing which one of these methods is more suitable requires a highly skilled anesthesiologist. By making use of these methods many of chronic and acute waist and neck IDH cases can be treated and also through physiotherapy and desirable exercises one can avoid surgeries.